The Environmental Press Model
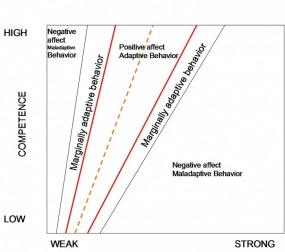
All information provided from: Christiansen, C. H. & Baum C. M. (2005). Occupational Therapy: Performance, Participation, and Well-Being.
This model is operationalized as the outcome of the transaction or interaction between the person and the environment. Optimal fit occurs when someone’s capacities are consistent with the demands / opportunities of within that person’s environment. However, if the demands of the environment exceed those of the person and their abilities, there is a person-environment misfit. This model can help key the treating therapist into determining the types of environmental changes that must be made in order to match the individual’s abilities.
The Y-axis of the graph depicts an individual’s competencies that are a result of their functional, biological, sensory/perceptual, cognitive, and social abilities as well as behavioral skills.
The X-axis represents the amount of environmental press or how accommodating their current environment is to their abilities.
Things to Consider in Regards to Jim:
Jim’s Y-Axis: Intrinsic Factors and Abilities
Functional: What tasks are currently difficult for Jim to perform?
Biological: Test functioning through ROM and manual muscle testing. What position hurts most / hurts least, etc.
Sensory/perceptual: Sensory deficits in his hands – temperature, light and heavy touch, paresthesias, numbness
Cognitive: There do not appear to be deficits in this area of function.
Social: How has the hand injury affected his social experience? Attending events? Being with friends?
Behavioral skills: How is Jim handling his situation? How does he feel about himself? How does he feel others perceive him?
Jim’s X-Axis: The Environment
The environment can be made up of 2 conceptualized terms: the physical and the psychosocial.
Physical:
His home environment: Investigate his living situation. A 2-story house. What does he do around the house – cook? What utensils does he use? Trouble opening containers? Opening doors? Typing on a computer – replying to emails, writing papers, reviewing notes, transcribing lectures, etc. Falls asleep studying before he can apply splint – where does he study, until when?
His environment at school: Opening doors, opening lockers, how does he take notes in class, does he carry around books, required to flip through papers, etc.
His work environment: What position does he sit in to dissect – what is he sitting on / when is he standing / what position is he doing these things in? What tools does he use? Can their handles be built up? Can the positions of the bodies be changed? When does he take breaks? Does he have anything to support his hand during this?
His community environment: How does he get to school – drive? When he goes out for drinks, how does he grip his glass? How does he carry grocery bags?
Psychosocial:
Consider the attitudes of those around them: housemates, friends, those in positions of authority, professors, strangers, health professionals, etc.
Compare the tasks Jim performs and how he performs them to the environmental support he currently has. Then ask:
What in the environment can be altered to help Jim?
What compensations can be made for Jim in order to help him function better in current living situations?
What adaptations can be provided to help him continue to participate in his roles, tasks, and activities?
Click Below to Go Back

